|
This rare case of MPT with heterologous liposarcomatous differentiation mimicking an intracystic tumor on sonography is presented with a review of the literature, pertinent imaging findings, and histopathological diagnostic criteria. This case demonstrates that all macroscopic fat-containing lesions on mammography are not benign. This was explored using other imaging modalities such as an ultrasound, breast MRI, and positron emission tomography (PET)–computed tomography (CT) scan. We present a histologically proven case of MPT with heterologous liposarcomatous transformation of the breast and that was found on a screening mammogram. The prior reports of these such masses mention their rarity however, they lack the discussion of imaging findings including correlation with breast magnetic resonance imaging (MRI). The finding of such a malignant heterologous element in PTs places the tumor into a malignant category. Patients with liposarcomatous differentiation, like in our case, may also develop as malignant differentiation of stromal components of PTs. 
Fatty lesions seen on mammograms and ultrasound tend to be either hamartoma or lipoma, with a malignant lesion thought of as a distant differential. 
MPTs carry a poor prognosis with an overall risk of local recurrence rates of 10%–40% and distant metastasis of 20%. Similarly, differentiation of the MPTs from spindle cell metaplastic carcinoma and primary breast sarcoma can also be challenging. Benign PT mimics fibroadenoma and their differentiation from malignant PT (MPT) is difficult on core biopsy. According to the World Health Organization (WHO), PTs are classified into benign, borderline, and malignant based on the histological features. Complete surgical removal with negative margin is the definitive treatment to avoid local recurrence. Malignant transformation of epithelial elements is very rare. Stromal component carries the high risk for the malignant transformation to usually fibrosarcomatous and rarely heterologous sarcomatous differentiation. The diagnosis of PTs requires histopathological confirmation of both epithelial and stromal components. PTs are common in 40–50 year age group and usually benign with malignant potential in up to 30% of cases. Other than seizures, most children are otherwise developing normally.Phyllodes tumors (PTs) are a rare fibroepithelial tumor of the breast which accounts for <1% of breast tumor and approximately 2%–3% of the breast fibroepithelial neoplasms. They can also be seen during daytime naps. They typically are seen shortly after the child goes to sleep or just before they wake up. Seizures that come on when the child is sleeping may start with twitching of one side of the face, but often progress to a generalized tonic-clonic seizure. These seizures are typically brief, lasting no more than 2 minutes in most cases, and are usually infrequent. These symptoms can interfere with speech and may cause drooling. 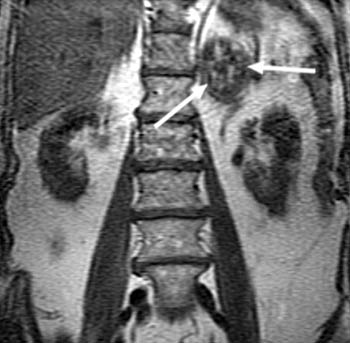
Seizures that begin during wakefulness involve twitching, numbness, or tingling of one side of the face or tongue. Seizures in CECTs can occur when the child is awake or during sleep. Yet, many people still just use the term benign rolandic epilepsy to refer to this syndrome. The official modern name is “childhood epilepsy with centrotemporal spikes” or CECTS. The term “benign” refers to the fact that most children outgrow these seizures by adolescence. The name derives from the rolandic area of the brain, which is the part that controls movements.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
